Osteochondritis Dissecans (OCD) is an acquired potentially reversible lesion of the subchondral bone which also affects the overlying cartilage. The causes of OCD are unknown. If OCD progresses, it can lead to articular cartilage instability. When OCD affects the knee, the most common location is within the lateral aspect of the medial femoral condyle. Juvenile OCD lesions have a better healing prognosis than adults. Generally, OCD seems to affect males more commonly than females (between 2:1 and 3:1). However, as females and younger children participate in sports there has been an increased prevalence among girls and a younger mean age of OCD onset.
Etiology/ Pathoanatomy
The causes of OCD are unknown, however repetitive trauma, inflammation, accessory centers of ossification, ischemia, and genetic factors show causative correlation. ). Some familial tendencies exist, but non-familial OCD is most prevalent. Repetitive trauma caused by year round sports, early sports specialization, multiple sports in a singe leason or multiple teams in a single sport and increased training intensity are some of the causative factor associated with OCD. Chronic repetitive microtrauma has been suggested to lead to a stress reaction within the subchondral bone and in more severe cases subchondral bone necrosis where fragment dissection and separation may ensue.
Evaluation
Patients with OCD of knee initially have nonspecific complaints, with anterior knee pain and variable amounts of intermittent swelling. With progression of the disease, patients may complain of more persistent swelling or effusion, catching, locking, and/or giving way. Unfortunately, pain and swelling are not good indicators of dissection. Physical findings may include a positive Wilson test, which reproduces the pain by internally rotating the tibia during extension of the knee between 90 and 30 degrees, then relieving the pain with tibial external rotation. The premise for this test is that the tibial eminence impinges on the OCD lesion in internal rotation and extension; whereas, external rotation moves the eminence away from the lesion.
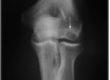
Standard weight-bearing radiographs of both knees are helpful for initially characterizing the lesion type and status of the growth plate. The lateral view helps identify anterior-posterior lesion location and normal, benign accessory ossification centers in the skeletally immature knee. An axial view is helpful if a lesion of the patella or trochlea is suspected, and a “notch view” in 30 to 50 degrees of knee flexion may help identify the lesions of the posterior femoral condyle.
Studies have been performed to attempt to identify specific MRI findings that link the ability of OCD lesions to heal following non-operative treatment.
Non-Operative Treatment
The goal of non-operative intervention is to promote healing in the subchondral bone and prevent chondral collapse, subsequent fracture, and crater formation. The treatment depends on skeletal maturity of the patient, as well as the size, stability, and location of the lesion as the more skeletally mature a patient, the worse the prognosis. Non-surgical treatment is the treatment of choice for small stable lesions in skeletally immature patients with wide open physes and no signs of instability on MRI. Nonsurgical management focuses on significant activity modification by limiting high impact activities. Short-term immobilization and protected weight bearing may be helpful. Alternatively, bracing and range-of-motion knee exercises may be beneficial. Typically a period of three to nine months of non-operative treatment is initiated. Surgical treatment to promote healing is suggested when non-surgical methods fail and for skeletally mature patients with large lesions.
Operative Treatment
Surgical management begins with arthroscopy . Operative treatment should be considered for patients with unstable or detached lesions, failed non-operative treatment, and for patients approaching skeletal maturity. The goals of operative treatment are to promote healing of subchondral bone, to maintain joint congruity, to fix rigidly unstable fragments, and to replace osteochondral defects with cells that can replace and grow cartilage. (53) Optimal surgical treatment provides a stable construct of subchondral bone, calcified tidemark, and repair cartilage with viability and biomechanical properties equivalent to or similar to native hyaline cartilage.
Surgical treatment for stable lesions with intact articular cartilage involves drilling the subchondral bone with the intention of stimulating vascular ingrowth and subchondral bone healing. If the lesion is unstable and hinged, fixation is indicated. For patients with a hinged lesion without subchondral support, bone grafting is indicated to restore articular congruency. The goal is to fix the osseous portion of the fragment to allow healing and stabilization of the overlying articular surface. Arthroscopic or open reduction and internal fixation can be performed with hardware using Kirschner wires, cannulated screws, or Herbert screws. Associated complications include implant migration, adjacent cartilage damage, and hardware fracture. Osteochondral plugs have recently been presented as a biologic alternative to the use of hardware. The plugs provide bone graft as well as fixation of the lesion (26,34)
If fixation is not possible, there are several salvage techniques for full-thickness defects, including marrow stimulation techniques such as microfracture as well as autologous chondrocyte implantation, and osteochondral autograft transplantation. However, these techniques have limited clinical outcome data in adolescents.
[toggle hide=”yes” border=”yes” style=”white” title_closed=”Open References” title_open=”Close References”]
References
1. Aglietti, P.; Buzzi, R.; Bassi, P. B.and Fioriti, M.: Arthroscopic drilling in juvenile osteochondritis dissecans of the medial femoral condyle. Arthroscopy, 10(3): 286-91, 1994.
2. Anderson, A. F.; Richards, D. B.; Pagnani, M. J.and Hovis, W. D.: Antegrade drilling for osteochondritis dissecans of the knee. Arthroscopy, 13(3): 319-24, 1997.
3. Cahill, B. R.and Berg, B. C.: 99m-Technetium phosphate compound joint scintigraphy in the management of juvenile osteochondritis dissecans of the femoral condyles. Am J Sports Med, 11(5): 329-35, 1983.
4. Cahill, B. R.: Osteochondritis Dissecans of the Knee: Treatment of Juvenile and Adult Forms. J Am Acad Orthop Surg, 3(4): 237-247, 1995.
5. De Smet, A. A.; Ilahi, O. A.and Graf, B. K.: Untreated osteochondritis dissecans of the femoral condyles: prediction of patient outcome using radiographic and MR findings. Skeletal Radiol, 26(8): 463-7, 1997.
6. Flynn, J.M. Kocher, M.S. Ganley, T.J. Osteochodritis Dissecans of the Knee. J. Pediatr. Orthop., 2004, Jul-Aug: 24(4): 434-43.
7. Ganley TJ, Flynn JM: Osteochondritis Dissecans. In: Insall &Scott Surgery of the Knee, Fourth Edition, Volume 2, Elsevier, 1234-1241, 2006.
8. Kocher, M. S., Micheli, L.J.; Yaniv, M.; Zurakowski, D.; Ames, A.; Adrignolo, A.A.: Functional and Radiographic Outcome of Juvenile Osteochondritis Dissecans of the Knee Treated with Transarticular Arthroscopic Drilling. Am J Sports Med, 29(5): 562-566, 2001.
9. Kocher MS, Tucker R, Ganley TJ, Flynn JM: Management of Osteochondritis Dissecans of the Knee: Current Concepts Review, American Journal of Sports Medicine, 2006 Jul;34(7): 1181-1191.
10. Peterson, L.; Minas, T.; Brittberg, M.and Lindahl, A.: Treatment of osteochondritis dissecans of the knee with autologous chondrocyte transplantation: results at two to ten years. J Bone Joint Surg Am, 85-A(Suppl 2): 17-24, 2003.
11. Pill, S. G.; Ganley, T. J.; Milam, R. A.; Lou, J. E.; Meyer, J. S.and Flynn, J. M.: Role of magnetic resonance imaging and clinical criteria in predicting successful nonoperative treatment of osteochondritis dissecans in children. J Pediatr Orthop, 23(1): 102-8, 2003.
12. O’Connor, M. A.; Palaniappan, M.; Khan, N.and Bruce, C. E.: Osteochondritis dissecans of the knee in children. A comparison of MRI and arthroscopic findings. J Bone Joint Surg Br, 84(2): 258-62, 2002.
13. Steadman, J.R.; Briggs, K.K.; Rodrigo, J.J.; Kocher, M.S.; Gill; T.J.; Rodkey, W.G.: Outcomes of microfracture for traumatic chondral defects of the knee: Average 11-year follow-up. Arthroscopy, 19(5): 477-484, 2003.
14. Thomson, N. L.: Osteochondritis dissecans and osteochondral fragments managed by Herbert compression screw fixation. Clin Orthop, (224): 71-8, 1987.
15. Twyman, R. S.; Desai, K.and Aichroth, P. M.: Osteochondritis dissecans of the knee. A long-term study. J Bone Joint Surg Br, 73(3): 461-4, 1991.
16. Vonstein, D. W. N., H. Laor, T. et al.: Juvenile Osteochondritis Dissecans of the Knee: Healing Prognosis Based on X-Ray and Gadolinium Enhanced MRI. Pediatric Orthopaedic Society of North America: 79, 2003.
17. Wilson, J. N.: A diagnostic sign in osteochondritis dissecans of the knee. J Bone Joint Surg Am, 49(3): 477-80, 1967.
18. Lefort G, Moyen B, Beaufils P, De Billy B, Breda R, Cadilhac C, Clavert p et al. Osteochondritis dissecans of the femoral condyles : report of 892 cases. Rev Chir Orthop Reparatrice Appar Mot. 2006 Sep; 92 (5 suppl): 97-141.
19. Din R, Annear P, Scadden J. Internal fixation of undisplaced lesions of osteochondritis dissecans in the knee. JBJS Br. 2006 Jul; 88(7): 900-4.
20. Micheli LJ, Moseley JB, Anderson AF, et al. Articular cartilage defects of the distal femur in children and adolescents : treatment with autologous chondrocyte implantation. J Pediatr Orthop. 2006 Jul-Aug; 26 (4): 455-460.
21. Krishnan SP, Skinner JA et al. Collagen-covered autologous chondrocyte implantation for osteochondritis dissecans of the knee: two to seven year results. JBJS Br. 2006 Feb; 88 (2): 203-5.
22. Makino A, Muscolo DL et al. Arthroscopic fixation of osteochondritis dissecans of the knee: clinical, magnetic resonance imagaging and arthroscopic follow-up. Am J Sports Med. 2005 Oct; 33 (10): 1499-504.
23. Gebarski K, Hernandez RJ. Stage-I osteochondritis dissecans versus normal variants of ossification in the knee in children. Pediatr Radiol. 2005 Sep; 35 (9): 880-6.
24. Uematsu K, Habata T, Hasegawa Y. Osteochondritis dissecans of the knee: long-term results of excision of the osteochondral fragments. Knee. 2005 Jun; 12 (3): 205-8.
25. Cepero S, ullot R, Sastre S. Osteochondritis of the femoral condyles in children and adolescents: our experience over the last 28 years. J Pediatr Orthop B. 2005 Jan; 14 (1): 24-9.
26. Kobayashi T, Fujikawa K, Oohashi M. Surgical fixation of massive osteochonritis dissecans lesion using cylindrical osteochondral plugs. Arthroscopy. 2004 Nov; 20 (9): 981-6.
27. Conrad JM, Stanitski CL. Osteochondritis dissecans: Wilson’s sign revisted. Am J Sports Med. 2003 Sep-Oct; 31 (5): 777-8.
28. Kawasaki K, Uchio Y, Adachi N, Iwasa J, Ochi M. Drilling from the intercondylar area for treatment of osteochondritis dissecans of the knee joint. Knee. 2003 Sep; 10 (3): 257-63.
29. Arnold CA, Thomas DJ, Sanders JO. Bilateral knee and bilateral elbow osteochondritis dissecans. Am J Orthop. 2003 May; 32 (5): 237 40.
30. Louisia S, Beaufils P et al. Transchondral drilling for osteochondritis dissecans of the medial condyle of the knee. Knee Surg Sports Traumatol Arthrosc. 2003 Jan; 11(1):33-39.
31. Lyle M, Curtis C et al. Articular Cartilage Repair in the Adolescent Athlete : Is Autologous Chondrocyte Implantation the Answer ? Clin J Sports Med. 2006 Nov. 16(6)
32. Linden B, Telhag H. Osteochondritis Dissecans. Acta orthop scand. 1977. 48, 682-686.
33. Murray JR, Chitnavis J et al. Osteochondritis dissecans of the knee; long term clinical outcome following. arthroscopic debridement. Knee. 2007 Jan 9.
34. Miniaci, Tytherleigh,Fixation of Unstable Knee OCDs Using Osteochondral Plugs. Arthroscopy 2007; 23(8): 845-851.
35. Fairbanks H. Osteochondritis Dissecans. JBJS Br. 1933; 21B: 67-82
36. Green WT, Banks HH. Osteochondritis dissecans in children. JBJS A. 1953; 35A: 26-47.
37. Petrie PW. Aetiology of osteochondritis dissecans: failure to establish a familial background. JBJSB 1977; 59: 366-367.
38. Bradley J, Dandy DJ. Results of drilling osteochondritis dissecans before skeletal maturity. JBJS Br 1989; 71B: 642-44.
39. Cahill BR, Phillips MR, Navarro R. The results of conservative management of juvenile osteochondritis dissecans using joint scintigraphy: a prospective study. Am J Sports Med 1989; 17: 601-606.
40. Clanton TO, DeLee JC. Osteochondritis dissecans: history, pathophysiology and current treatment concepts. Clin Orthop Relat Res 1982; 167: 50-64
41. Glancy GL. Juvenile osteochonritis dissecans. Am J Knee Surg 1999; 12: 120-124.
42. Green WT, Banks HH. Osteochondritis dissecans in children. JBJS A 1953; 35A: 26-47.
43. Hefti F, Beguiristain J, Krauspe R, et al. Osteochondritis dissecans: a multicenter study of the European Pediatric Orthopaedic Society. J Pediatr Orthop B 1999; 8: 231-245.
44. Kocher MS, Micheli LJ, Yaniv M, et al. Functional and radiographic outcome of juvenile osteochondritis dissecans of the knee treated with transarticular arthroscopic drilling. Am J Sports Med 2001; 29: 562-566.
45. Ribbing S. The hereditary multiple epiphyseal disturbance and its consequences for aetiogenesis of local malacias, particularly the osteochondrosis dissecans. Acta Orthop Scand 1955; 24: 286-299.
46. Bradley J, Dandy DJ. Results of drilling osteochondritis dissecans before skeletal maturity. JBJS Br. 1989; 71B: 642-644.
47. Aglietti P, Buzzi R, Bassi PB, et al. Arthroscopic drilling in juvenile osteochondritis dissecans of the medial femoral condyle. Arthroscopy 1994; 10: 286-291.
48. Kocher MS, Micheli LJ, Yaniv M, et al. Functional and radiographic outcome of juvenile osteochondritis dissecans of the knee treated with transarticular arthroscopic drilling. Am J Sports Med 2001; 29: 562-566.
49. DeSmet AA, Ilahi OA, Graf BK. Untreated osteochonritis dissecans of the femoral condyles : Prediction of patient outcome using radiographic and MR findings. Skeletal Radiol 26: 463-467, 1997.
50. Mubarak SJ, Carroll NC. Familial Osteochondritis Dissecans of the Knee. Clin Orthop Relat Res. 1979 May; (140): 131-6.
51. Wall EJ, Vourazeris J, Myer GD, Emergy KH, Divine JF, Nick TG, Hewett TE. The healing potential of stable juvenile osteochondritis dissecans knee lesions. JBJS A. 2008 Dec; 90 (12): 2655-64.
52. Bohndorf K. osteochondritis (osteochondrosis) dissecans: a review and new MRI classification. Eur Radiol. 1998; : 103-112.
53. Smillie I: Treatment of osteochondritis dissecans. J Bone Joint Surg Br 39:248-260, 1957.
54. Micheli L, Curtis C, Shervin, N, Articular Cartilage Repair in the Adolescent Athlete: Is Autologous Chondrocyte Implantation the Answer? Clin J Sport Med 16: 465-470.
[/toggle]